Bipolar disorder affects more than 5 million Americans each year. Despite its prevalence, bipolar disorder is still widely misunderstood. This mood disorder can cause mood swings, but also significant shifts in cognition, behavior, and emotions. Bipolar disorder can cause widespread consequences, including professional and personal conflicts, increased risk of suicide, and addiction. In this article, we’ll cover the relationship between bipolar disorder and addiction, background on the condition and the different treatment options available to you.
Contents
What Is Bipolar Disorder?
As with other mental health conditions, such as depression, anxiety, and affective disorders, bipolar disorder (formerly known as manic depression) is both a disorder and umbrella term referring to a collection of different conditions. People with bipolar disorder cycle through manic and depressed states in a short period of time— usually a few days or weeks.
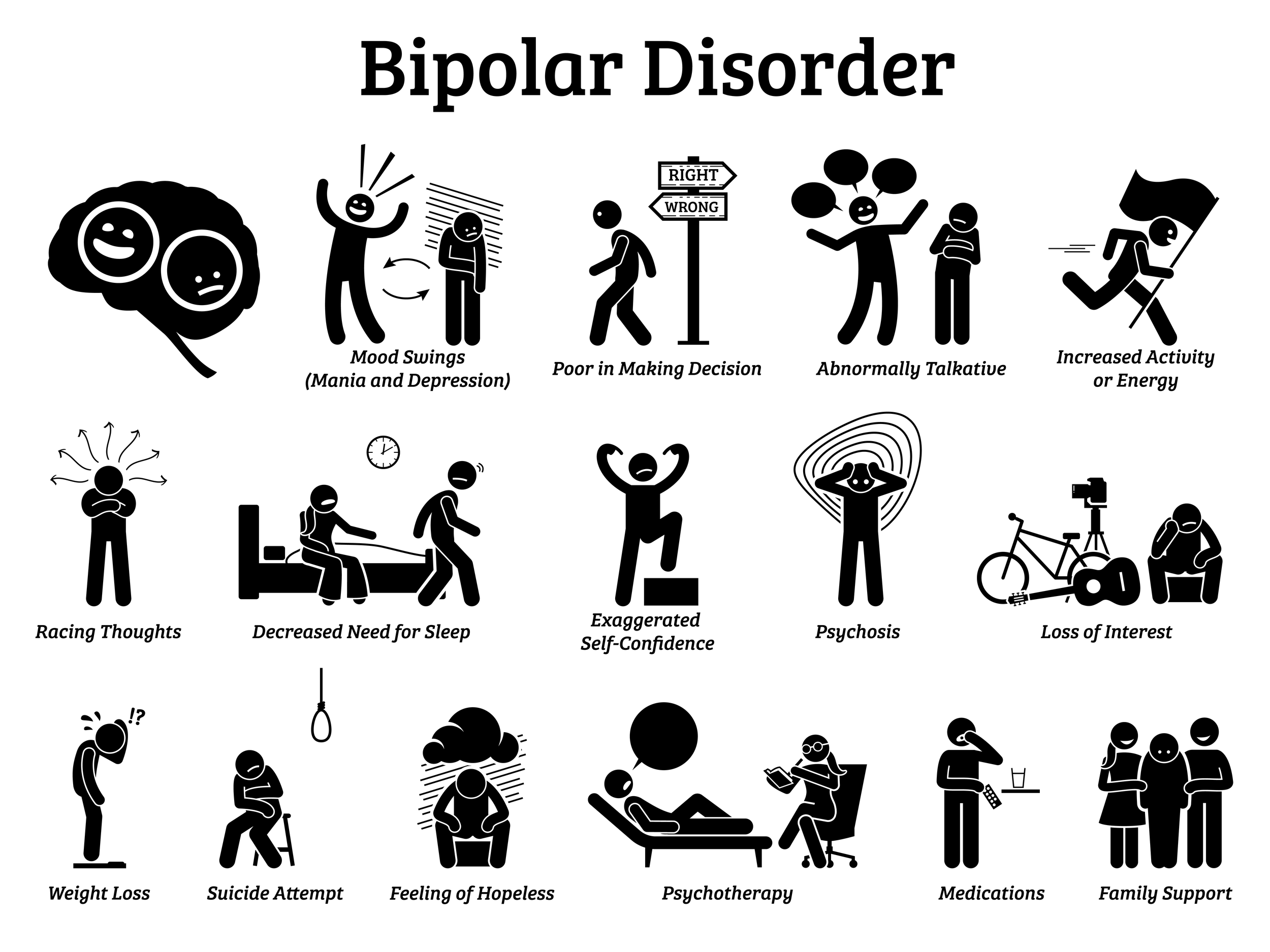
During manic episodes, you may feel boundless, uncontrollable energy accompanied by anxiety, sleep disturbances, and irritability. On the other hand, depressive episodes may cause you to feel lethargy, hopelessness, disinterest in activities, sleepy, and suicidal. In order for a doctor to diagnose you with this condition, you must suffer from at least one manic episode in a given period of time. Although you don’t need to have experienced a depressive episode, it is extremely common to have them as well.
What Are The Types of Bipolar Disorder?
There are several different subsets of bipolar disorder. However, thinking about this condition as a “bipolar spectrum” can be helpful for people who don’t feel like they fit into a particular diagnosis. Knowing the major classifications of the condition can still help you. The major types of bipolar disorder include:
Bipolar I Disorder
People with a Bipolar Disorder Type 1 (Bipolar I) diagnosis have experienced at least one manic episode. During these periods of extremely high energy, they may engage in reckless behaviors that are dangerous to themselves and those around them. In severe cases, they may even suffer from psychotic symptoms, including delusions and hallucinations that require hospitalization.
Bipolar II Disorder
Bipolar Disorder Type 2 (Bipolar II) is characterized by hypomanic episodes. Hypomania is a lower stage of a manic episode, where people experience increased energy levels, optimism, and even happiness. Because of these “positive” symptoms, individuals may not recognize they are suffering from bipolar disorder. People with bipolar II also tend to experience depressive episodes and face anxiety, irritability, or other problems that require medical attention.
Rapid Cycling Bipolar Disorder
Patients with bipolar disorder suffer from shifts in mood states. For those with rapid cycling bipolar disorder, these episodes happen more quickly—often within a week or two. This can cause a great disruption in everyday activities.
Furthermore, cycling through episodes that quickly may also be a sign of a personality disorder or other serious mental illness. In either case, be sure to seek medical attention immediately. Oftentimes, individuals with rapid cycling bipolar disorder are at a higher risk for dangerous behavior.
These are just three of the main types of bipolar disorder. Other common conditions include cyclothymic disorder and mixed episode bipolar disorder.
What Is the Relationship Between Bipolar Disorder and Substance Abuse?
Generally speaking, the link between mental illness and substance use disorder is very strong. However, those with bipolar disorder may have even higher rates of addiction than those with other mental health conditions. Nearly 40% of patients with bipolar I suffer from alcohol or drugs abuse.
Overall, there is a tendency for patients to self-medicate in order to alleviate their pain from the disorder. Common symptoms of bipolar disorder include:
- insomnia
- depression
- anxiety
- pain
Consequently, many people turn to drugs and alcohol to reduce discomfort. However, drug and alcohol abuse may actually trigger depressive and manic episodes. This can create a vicious downward cycle.
Age and gender also impact the development of addiction. For example, young men have a higher likelihood of engaging in substance abuse and reckless behaviors compared to other populations. Finally, brain chemistry may also play a role. People with abnormal dopamine, norepinephrine, and serotonin levels may be more likely to develop a co-occurring disorder.
Co-occurring drug or alcohol addiction only magnifies the negative outcomes of bipolar disorder. For this reason, individuals should seek a combination of therapies that targeting both bipolar disorder and addiction.
What Are the Warning Signs?
One dangerous aspect of co-occurring bipolar disorder and addiction is that can worsen the most intense aspects of both conditions. Individuals suffering from both bipolar and substance use disorder may:
- Experience more dramatic mood shifts
- Engage in reckless and dangerous behaviors
- Have emotional and violent outbursts
- Alternate more rapidly between mood states
- Be at a higher risk for suicide
However, these warning signs can lead to more severe symptoms. If you or someone you care about suffers from bipolar disorder, you should know the signs of drug and alcohol abuse.
What Is the Treatment for Bipolar Disorder and Addiction?
In the past, co-occurring disorders were usually treated separately. Oftentimes, people diagnosed with bipolar disorder were sent to mental health facilities. Meanwhile, those addicted to drugs or alcohol were sent to rehab centers. Unfortunately, this separation led to higher rates of relapse and less effective treatment strategies.

Nowadays, clinicians treat both conditions simultaneously through the process of “integrated treatment.” During integrated treatment, your care involves numerous components designed to help address your co-occurring disorders. This generally involves a combination of individual and group therapy, family counseling, medical detox, and other strategies. Usually, integrated treatment includes the following features:
- Interdisciplinary treatment through a care team, including mental health professionals, social workers, nurses, support staff, and others
- Centralized care in a single facility
- Cognitive-behavioral therapy focused on managing emotions and reducing substance abuse
- Medication to regulate mood states caused by bipolar disorder
- Relapse prevention strategies
- Peer support from others battling co-occurring bipolar disorder and addiction
Substance abuse and bipolar disorder should be treated together. This type of care is called dual diagnosis. Without comprehensive care, there is a much higher chance of relapse. Ultimately, patients need a way to be equipped with many skills. This includes methods to manage their emotions and triggers, as well as thrive in any environment.
The Dual Diagnosis Therapeutical Approach
Dual diagnosis patients need to learn how to regulate their emotions to manage their significant mood shifts. One of the key tools is group therapy. Here, patients can learn about common triggers and risk factors in an open, supportive environment.
Moreover, clinicians often tailor either a cognitive-behavioral therapeutic or a dialectical behavioral therapeutic approach. These different methods help patients understand what’s happening to them in better detail and give ways to move forward. Many patients may also be prescribed mood-stabilizing medication or antidepressants to provide additional support for their recovery.
Overcoming Bipolar Disorder and Addiction
Co-occurring bipolar disorder and addiction are extremely serious. Many of these individuals may engage in dangerous behaviors, act violent, and have severe disruptions in their everyday lives. However, through dual diagnosis treatment, it is possible to overcome both conditions and to get the necessary help. If you or a loved one are suffering from co-occurring disorders, make sure to seek guidance from a mental health professional right away.
We Can Help You
Port St. Lucie Hospital specializes in mental health services and is located on 20 acres near the beautiful Savannas Preserve. If you or one of your loved ones is struggling with a mental health disorder, we can help. Our 24-hour mental health services are provided by licensed professionals in various disciplines. We tailor our programs to our patient’s needs and will help you every step of the way.
We welcome you to our facility. From support groups to individual therapy treatment options, we are here to fight the battle with you. Reach out to us online today. You can also call us at (772) 335-0400.